TRECATOR®
(ethionamide)
Find TRECATOR® medical information:
Find TRECATOR® medical information:
TRECATOR® Quick Finder
Indications and Usage
INDICATIONS AND USAGE
Trecator is primarily indicated for the treatment of active tuberculosis in patients with M. tuberculosis resistant to isoniazid or rifampin, or when there is intolerance on the part of the patient to other drugs. Its use alone in the treatment of tuberculosis results in the rapid development of resistance. It is essential, therefore, to give a suitable companion drug or drugs, the choice being based on the results of susceptibility tests. If the susceptibility tests indicate that the patient's organism is resistant to one of the first-line anti-tuberculosis drugs (i.e., isoniazid or rifampin) yet susceptible to ethionamide, ethionamide should be accompanied by at least one drug to which the M. tuberculosis isolate is known to be susceptible.3 If the tuberculosis is resistant to both isoniazid and rifampin, yet susceptible to ethionamide, ethionamide should be accompanied by at least two other drugs to which the M. tuberculosis isolate is known to be susceptible.3
To reduce the development of drug-resistant bacteria and maintain the effectiveness of Trecator and other antibacterial drugs, Trecator should be used only to treat infections that are proven or strongly suspected to be caused by susceptible bacteria. When culture and susceptibility information are available, they should be considered in selecting or modifying antibacterial therapy. In the absence of such data, local epidemiology and susceptibility patterns may contribute to the empiric selection of therapy.
Patient nonadherence to prescribed treatment can result in treatment failure and in the development of drug-resistant tuberculosis, which can be life-threatening and lead to other serious health risks. It is, therefore, essential that patients adhere to the drug regimen for the full duration of treatment. Directly observed therapy is recommended for all patients receiving treatment for tuberculosis. Patients in whom drug-resistant M. tuberculosis organisms are isolated should be managed in consultation with an expert in the treatment of drug-resistant tuberculosis.
Dosage and Administration
DOSAGE AND ADMINISTRATION
In the treatment of tuberculosis, a major cause of the emergence of drug-resistant organisms, and thus treatment failure, is patient nonadherence to prescribed treatment. Treatment failure and drug-resistant organisms can be life-threatening and may result in other serious health risks. It is, therefore, important that patients adhere to the drug regimen for the full duration of treatment. Directly observed therapy is recommended when patients are receiving treatment for tuberculosis. Consultation with an expert in the treatment of drug-resistant tuberculosis is advised for patients in whom drug-resistant tuberculosis is suspected or likely. Ethionamide should be administered with at least one, sometimes two, other drugs to which the organism is known to be susceptible (see INDICATIONS AND USAGE).
Trecator is administered orally. The usual adult dose is 15 to 20 mg/kg/day, administered once daily or, if patient exhibits poor gastrointestinal tolerance, in divided doses, with a maximum daily dosage of 1 gram.
Trecator tablets have been reformulated from a sugar-coated tablet to a film-coated tablet. Patients should be monitored and have their dosage retitrated when switching from the sugar-coated tablet to the film-coated tablet (see CLINICAL PHARMACOLOGY).
Therapy should be initiated at a dose of 250 mg daily, with gradual titration to optimal doses as tolerated by the patient. A regimen of 250 mg daily for 1 or 2 days, followed by 250 mg twice daily for 1 or 2 days with a subsequent increase to 1 gm in 3 or 4 divided doses has been reported.4,5 Thus far, there is insufficient evidence to indicate the lowest effective dosage levels. Therefore, in order to minimize the risk of resistance developing to the drug or to the companion drug, the principle of giving the highest tolerated dose (based on gastrointestinal intolerance) has been followed. In the adult this would seem to be between 0.5 and 1.0 gm daily, with an average of 0.75 gm daily.
The optimum dosage for pediatric patients has not been established. However, pediatric dosages of 10 to 20 mg/kg p.o. daily in 2 or 3 divided doses given after meals or 15 mg/kg/24 hrs as a single daily dose have been recommended.1,2 As with adults, ethionamide may be administered to pediatric patients once daily. It should be noted that in patients with concomitant tuberculosis and HIV infection, malabsorption syndrome may be present. Drug malabsorption should be suspected in patients who adhere to therapy, but who fail to respond appropriately. In such cases, consideration should be given to therapeutic drug monitoring (see CLINICAL PHARMACOLOGY).
The best times of administration are those which the individual patient finds most suitable in order to avoid or minimize gastrointestinal intolerance, which is usually at mealtimes. Every effort should be made to encourage patients to persevere with treatment when gastrointestinal side effects appear, since they may diminish in severity as treatment proceeds.
Concomitant administration of pyridoxine is recommended.
Duration of treatment should be based on individual clinical response. In general, continue therapy until bacteriological conversion has become permanent and maximal clinical improvement has occurred.
Contraindications
Warnings and Precautions
WARNINGS
The use of Trecator alone in the treatment of tuberculosis results in rapid development of resistance. It is essential, therefore, to give a suitable companion drug or drugs, the choice being based on the results of susceptibility testing. However, therapy may be initiated prior to receiving the results of susceptibility tests as deemed appropriate by the physician. Ethionamide should be administered with at least one, sometimes two, other drugs to which the organism is known to be susceptible (see INDICATIONS AND USAGE). Drugs which have been used as companion agents are rifampin, ethambutol, pyrazinamide, cycloserine, kanamycin, streptomycin, and isoniazid. The usual warnings, precautions, and dosage regimens for these companion drugs should be observed.
Patient compliance is essential to the success of the anti-tuberculosis therapy and to prevent the emergence of drug-resistant organisms. Therefore, patients should adhere to the drug regimen for the full duration of treatment. It is recommended that directly observed therapy be practiced when patients are receiving anti-tuberculous medication. Additional consultation from experts in the treatment of drug-resistant tuberculosis is recommended when patients develop drug-resistant organisms.
Severe Cutaneous Adverse Reactions
Cases of severe cutaneous adverse reactions (SCARs), such as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), and acute generalized exanthematous pustulosis (AGEP) have been reported with the use of combinations of anti-tuberculosis drugs that included ethionamide (see ADVERSE REACTIONS). If symptoms or signs of SCARs develop, discontinue suspect drug(s) immediately and institute appropriate therapy.
PRECAUTIONS
General
Prescribing Trecator in the absence of a proven or strongly suspected bacterial infection indication is unlikely to provide benefit to the patient and increases the risk of the development of drug-resistant bacteria.
Ethionamide may potentiate the adverse effects of the other anti-tuberculous drugs administered concomitantly (see Drug Interactions). Ophthalmologic examinations (including ophthalmoscopy) should be performed before and periodically during therapy with Trecator.
Information For Patients
Patients should be advised to consult their physician should blurred vision or any loss of vision, with or without eye pain, occur during treatment.
Excessive ethanol ingestion should be avoided because a psychotic reaction has been reported.
Patients should be counseled that antibacterial drugs including Trecator should only be used to treat bacterial infections. They do not treat viral infections (e.g., the common cold). When Trecator is prescribed to treat a bacterial infection, patients should be told that although it is common to feel better early in the course of therapy, the medication should be taken exactly as directed. Skipping doses or not completing the full course of therapy may (1) decrease the effectiveness of the immediate treatment and (2) increase the likelihood that bacteria will develop resistance and will not be treatable by Trecator or other antibacterial drugs in the future.
Laboratory Tests
Determination of serum transaminases (SGOT, SGPT) should be made prior to initiation of therapy and should be monitored monthly. If serum transaminases become elevated during therapy, ethionamide and the companion anti-tuberculosis drug or drugs may be discontinued temporarily until the laboratory abnormalities have resolved. Ethionamide and the companion anti-tuberculosis medication(s) then should be reintroduced sequentially to determine which drug (or drugs) is (are) responsible for the hepatotoxicity.
Blood glucose determinations should be made prior to and periodically throughout therapy with Trecator. Diabetic patients should be particularly alert for episodes of hypoglycemia.
Periodic monitoring of thyroid function tests is recommended as hypothyroidism, with or without goiter, has been reported with ethionamide therapy.
Drug Interactions
Trecator has been found to temporarily raise serum concentrations of isoniazid. Trecator may potentiate the adverse effects of other anti-tuberculous drugs administered concomitantly. In particular, convulsions have been reported when ethionamide is administered with cycloserine and special care should be taken when the treatment regimen includes both of these drugs. Excessive ethanol ingestion should be avoided because a psychotic reaction has been reported.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Teratogenic Effects
Animal studies conducted with Trecator indicate that the drug has teratogenic potential in rabbits and rats. The doses used in these studies on a mg/kg basis were considerably in excess of those recommended in humans. There are no adequate and well-controlled studies in pregnant women. Because of these animal studies, however, it must be recommended that Trecator be withheld from women who are pregnant, or who are likely to become pregnant while under therapy, unless the prescribing physician considers it to be an essential part of the treatment.
Nursing Mothers
Because no information is available on the excretion of ethionamide in human milk, Trecator should be administered to nursing mothers only if the benefits outweigh the risks. Newborns who are breast-fed by mothers who are taking Trecator should be monitored for adverse effects.
Pediatric Use
Due to the fact that pulmonary tuberculosis resistant to primary therapy is rarely found in neonates, infants, and children, investigations have been limited in these age groups. At present, the drug should not be used in pediatric patients under 12 years of age except when the organisms are definitely resistant to primary therapy and systemic dissemination of the disease, or other life-threatening complications of tuberculosis, is judged to be imminent.
Adverse Reactions
ADVERSE REACTIONS
Gastrointestinal
The most common side effects of ethionamide are gastrointestinal disturbances including nausea, vomiting, diarrhea, abdominal pain, excessive salivation, metallic taste, stomatitis, anorexia and weight loss. Adverse gastrointestinal effects appear to be dose related, with approximately 50% of patients unable to tolerate 1 gm as a single dose. Gastrointestinal effects may be minimized by decreasing dosage, by changing the time of drug administration, or by the concurrent administration of an antiemetic agent.
Nervous System
Psychotic disturbances (including mental depression), drowsiness, dizziness, restlessness, headache, and postural hypotension have been reported with ethionamide. Rare reports of peripheral neuritis, optic neuritis, diplopia, blurred vision, and a pellagra-like syndrome also have been reported. Concurrent administration of pyridoxine has been recommended to prevent or relieve neurotoxic effects.
Other
Hypersensitivity reactions including rash, photosensitivity, thrombocytopenia and purpura have been reported rarely. Hypoglycemia, hypothyroidism, gynecomastia, impotence, and acne also have occurred. The management of patients with diabetes mellitus may become more difficult in those receiving ethionamide.
Immune System Disorders: SCARs such as SJS, TEN, DRESS, and AGEP have been reported with the use of combinations of anti-tuberculosis drugs that included ethionamide (see WARNINGS).
Overdosage
Description
DESCRIPTION
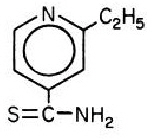
Trecator (ethionamide tablets, USP) is used in the treatment of tuberculosis. The chemical name for ethionamide is 2-ethylthioisonicotinamide with the following structural formula:
Ethionamide is a yellow crystalline, nonhygroscopic compound with a faint to moderate sulfide odor and a melting point of 162°C. It is practically insoluble in water and ether, but soluble in methanol and ethanol. It has a partition coefficient (octanol/water) Log P value of 0.3699. Trecator tablets contain 250 mg of ethionamide. The inactive ingredients present are croscarmellose sodium, FD&C Yellow #6, magnesium stearate, microcrystalline cellulose, polyethylene glycol, polyvinyl alcohol, povidone, silicon dioxide, talc, and titanium dioxide.
Clinical Pharmacology
CLINICAL PHARMACOLOGY
Absorption
Ethionamide is essentially completely absorbed following oral administration and is not subjected to any appreciable first pass metabolism. Ethionamide tablets may be administered without regard to the timing of meals.
The pharmacokinetic parameters of ethionamide following single oral-dose administration of 250 mg of Trecator film-coated tablets under fasted conditions to 40 healthy adult volunteers are provided in Table 1.
| Cmax (µg/mL) | Tmax (hrs) | AUC (µg∙hr/mL) | |
|---|---|---|---|
Film-Coated Tablet | 2.16 | 1.02 | 7.67 |
Trecator tablets have been reformulated from a sugar-coated tablet to a film-coated tablet. The Cmax for the film-coated tablets (2.16 µg/mL) was significantly higher than that of sugar-coated tablets (1.48 µg/mL) (see DOSAGE AND ADMINISTRATION).
Distribution
Ethionamide is rapidly and widely distributed into body tissues and fluids following administration of a sugar-coated tablet, with concentrations in plasma and various organs being approximately equal. Significant concentrations are also present in cerebrospinal fluid following administration of a sugar-coated tablet. Distribution of ethionamide into the same body tissues and fluids, including cerebrospinal fluid following administration of the film-coated tablet, has not been studied, but is not expected to differ significantly from that of the sugar-coated tablet. The drug is approximately 30% bound to proteins. The mean (SD) apparent oral volume of distribution observed in 40 healthy volunteers following a 250 mg oral dose of film-coated tablets was 93.5 (19.2) L.
Metabolism
Ethionamide is extensively metabolized to active and inactive metabolites. Metabolism is presumed to occur in the liver and thus far 6 metabolites have been isolated: 2-ethylisonicotinamide, carbonyl-dihydropyridine, thiocarbonyl-dihydropyridine, S-oxocarbamoyl dihydropyridine, 2-ethylthioiso-nicotinamide, and ethionamide sulphoxide. The sulphoxide metabolite has been demonstrated to have antimicrobial activity against Mycobacterium tuberculosis.
Elimination
The mean (SD) half-life observed in 40 healthy volunteers following a 250 mg oral dose of film-coated tablets was 1.92 (0.27) hours. Less than 1% of the oral dose is excreted as ethionamide in urine.
Mechanism of Action
Ethionamide may be bacteriostatic or bactericidal in action, depending on the concentration of the drug attained at the site of infection and the susceptibility of the infecting organism. The exact mechanism of action of ethionamide has not been fully elucidated, but the drug appears to inhibit peptide synthesis in susceptible organisms.
Microbiology
In Vitro Activity
Ethionamide exhibits bacteriostatic activity against extracellular and intracellular Mycobacterium tuberculosis organisms. The development of ethionamide resistant M. tuberculosis isolates can be obtained by repeated subculturing in liquid or on solid media containing increasing concentrations of ethionamide. Multi-drug resistant strains of M. tuberculosis may have acquired resistance to both isoniazid and ethionamide. However, the majority of M. tuberculosis isolates that are resistant to one are usually susceptible to the other. There is no evidence of cross-resistance between ethionamide and para-aminosalicylic acid (PAS), streptomycin, or cycloserine. However, limited data suggest that cross-resistance may exist between ethionamide and thiosemicarbazones (i.e., thiacetazone) as well as isoniazid.
In Vivo Activity
Ethionamide administered orally initially decreased the number of culturable Mycobacterium tuberculosis organisms from the lungs of H37Rv infected mice. Drug resistance developed with continued ethionamide monotherapy, but did not occur when mice received ethionamide in combination with streptomycin or isoniazid.
References
REFERENCES
- 1.
- Feigin, R.D., and Cherry, J.D.: Textbook of Pediatric Infectious Diseases, 2nd Edition. Philadelphia, W.B. Saunders Co., 1987, pp. 1371–1372.
- 2.
- Nelson, W.E., Behrman, R.E., Vaughan, V.C. (eds.): Nelson Textbook of Pediatrics, 13th edition. Philadelphia, W.B. Saunders Co., 1987, p.636.
- 3.
- Treatment of Tuberculosis and Tuberculosis Infection in Adults and Children, Am J Respiratory and Critical Care Medicine, 149:1359–1374, 1994.
- 4.
- Peloquin, CA: Pharmacology of the Antimycobacterial Drugs, Med Clin North Am 77(6): 1230–1262, 1993.
- 5.
- American Thoracic Society. Am J Respir Crit Care Med 1997;156:S1–S25.
How Supplied/Storage and Handling
Other
Resources
Didn’t find what you were looking for?
Contact us.
Chat online with Pfizer Medical Information regarding your inquiry on a Pfizer medicine.
*Speak with a Pfizer Medical Information Professional regarding your medical inquiry. Available 9AM-5Pm ET Monday to Friday; excluding holidays.
Submit a medical question for Pfizer prescription products.
Report Adverse Event
To report an adverse event related to a Pfizer product and you are not part of a clinical trial* for this product, click the link below to submit your information: Pfizer Safety Reporting Site
*If you are involved in a clinical trial for either product, adverse events should be reported to your coordinating study site.
If you cannot use the above website to report an adverse event related to a Pfizer product, please call Pfizer Medical Information at (800) 438-1985.
You may also contact the U.S. Food and Drug Administration (FDA) directly to report adverse events or product quality concerns either online at www.fda.gov/medwatch or by calling (800)-332-1088.