AZTREONAM Clinical Pharmacology
(aztreonam for injection, USP)
CLINICAL PHARMACOLOGY
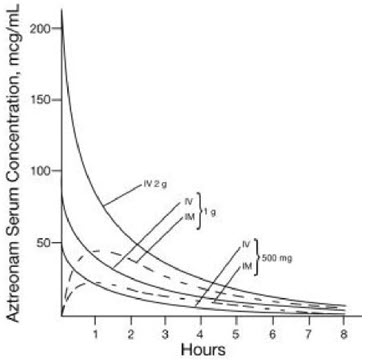
Single 30-minute intravenous infusions of 500 mg, 1 g, and 2 g doses of aztreonam for injection in healthy subjects produced aztreonam peak serum levels of 54 mcg/mL, 90 mcg/mL, and 204 mcg/mL, respectively, immediately after administration; at 8 hours, serum levels were 1 mcg/mL, 3 mcg/mL, and 6 mcg/mL, respectively (Figure 1). Single 3-minute intravenous injections of the same doses resulted in serum levels of 58 mcg/mL, 125 mcg/mL, and 242 mcg/mL at 5 minutes following completion of injection.
Serum concentrations of aztreonam in healthy subjects following completion of single intramuscular injections of 500 mg and 1 g doses are depicted in Figure 1; maximum serum concentrations occur at about 1 hour. After identical single intravenous or intramuscular doses of aztreonam for injection, the serum concentrations of aztreonam are comparable at 1 hour (1.5 hours from start of intravenous infusion) with similar slopes of serum concentrations thereafter.
 |
The serum levels of aztreonam following single 500 mg or 1 g (intramuscular or intravenous) or 2 g (intravenous) doses of aztreonam for injection exceed the MIC90 for Neisseria sp., Haemophilus influenzae, and most genera of the Enterobacteriaceae for 8 hours (for Enterobacter sp., the 8-hour serum levels exceed the MIC for 80% of strains). For Pseudomonas aeruginosa, a single 2 g intravenous dose produces serum levels that exceed the MIC90 for approximately 4 to 6 hours. All of the above doses of aztreonam for injection result in average urine levels of aztreonam that exceed the MIC90 for the same pathogens for up to 12 hours.
When aztreonam pharmacokinetics were assessed for adult and pediatric patients, they were found to be comparable (down to 9 months old). The serum half-life of aztreonam averaged 1.7 hours (1.5 to 2) in subjects with normal renal function, independent of the dose and route of administration. In healthy subjects, based on a 70 kg person, the serum clearance was 91 mL/min and renal clearance was 56 mL/min; the apparent mean volume of distribution at steady-state averaged 12.6 liters, approximately equivalent to extracellular fluid volume.
In elderly patients, the mean serum half-life of aztreonam increased and the renal clearance decreased, consistent with the age-related decrease in creatinine clearance. The dosage of aztreonam for injection should be adjusted accordingly (see DOSAGE AND ADMINISTRATION: Renal Impairment in Adult Patients).
In patients with impaired renal function, the serum half-life of aztreonam is prolonged (see DOSAGE AND ADMINISTRATION: Renal Impairment in Adult Patients). The serum half-life of aztreonam is only slightly prolonged in patients with hepatic impairment since the liver is a minor pathway of excretion.
Average urine concentrations of aztreonam were approximately 1,100 mcg/mL, 3,500 mcg/mL, and 6,600 mcg/mL within the first 2 hours following single 500 mg, 1 g, and 2 g intravenous doses of aztreonam for injection (30-minute infusions), respectively. The range of average concentrations for aztreonam in the 8- to 12-hour urine specimens in these studies was 25 to 120 mcg/mL. After intramuscular injection of single 500 mg and 1 g doses of aztreonam for injection, urinary levels were approximately 500 mcg/mL and 1,200 mcg/mL, respectively, within the first 2 hours, declining to 180 mcg/mL and 470 mcg/mL in the 6- to 8-hour specimens. In healthy subjects, aztreonam is excreted in the urine about equally by active tubular secretion and glomerular filtration. Approximately 60% to 70% of an intravenous or intramuscular dose was recovered in the urine by 8 hours. Urinary excretion of a single parenteral dose was essentially complete by 12 hours after injection. About 12% of a single intravenous radiolabeled dose was recovered in the feces. Unchanged aztreonam and the inactive beta-lactam ring hydrolysis product of aztreonam were present in feces and urine.
Intravenous or intramuscular administration of a single 500 mg or 1 g dose of aztreonam for injection every 8 hours for 7 days to healthy subjects produced no apparent accumulation of aztreonam or modification of its disposition characteristics; serum protein binding averaged 56% and was independent of dose. An average of about 6% of a 1 g intramuscular dose was excreted as a microbiologically inactive open beta-lactam ring hydrolysis product (serum half-life approximately 26 hours) of aztreonam in the 0- to 8-hour urine collection on the last day of multiple dosing.
Renal function was monitored in healthy subjects given aztreonam; standard tests (serum creatinine, creatinine clearance, BUN, urinalysis, and total urinary protein excretion) as well as special tests (excretion of N-acetyl-β-glucosaminidase, alanine aminopeptidase, and β2-microglobulin) were used. No abnormal results were obtained.
Aztreonam achieves measurable concentrations in the following body fluids and tissues:
| Fluid or Tissue | Dose (g) | Route | Hours Post-injection | Number of Patients | Mean Concentration (mcg/mL or mcg/g) |
|---|---|---|---|---|---|
| |||||
| Fluids | |||||
| bile | 1 | IV | 2 | 10 | 39 |
| blister fluid | 1 | IV | 1 | 6 | 20 |
| bronchial secretion | 2 | IV | 4 | 7 | 5 |
| cerebrospinal fluid (inflamed meninges) | 2 | IV | 0.9 to 4.3 | 16 | 3 |
| pericardial fluid | 2 | IV | 1 | 6 | 33 |
| pleural fluid | 2 | IV | 1.1 to 3 | 3 | 51 |
| synovial fluid | 2 | IV | 0.8 to 1.9 | 11 | 83 |
| Tissues | |||||
| atrial appendage | 2 | IV | 0.9 to 1.6 | 12 | 22 |
| endometrium | 2 | IV | 0.7 to 1.9 | 4 | 9 |
| fallopian tube | 2 | IV | 0.7 to 1.9 | 8 | 12 |
| fat | 2 | IV | 1.3 to 2 | 10 | 5 |
| femur | 2 | IV | 1 to 2.1 | 15 | 16 |
| gallbladder | 2 | IV | 0.8 to 1.3 | 4 | 23 |
| kidney | 2 | IV | 2.4 to 5.6 | 5 | 67 |
| large intestine | 2 | IV | 0.8 to 1.9 | 9 | 12 |
| liver | 2 | IV | 0.9 to 2 | 6 | 47 |
| lung | 2 | IV | 1.2 to 2.1 | 6 | 22 |
| myometrium | 2 | IV | 0.7 to 1.9 | 9 | 11 |
| ovary | 2 | IV | 0.7 to 1.9 | 7 | 13 |
| prostate | 1 | IM | 0.8 to 3 | 8 | 8 |
| skeletal muscle | 2 | IV | 0.3 to 0.7 | 6 | 16 |
| skin | 2 | IV | 0 to 1 | 8 | 25 |
| sternum | 2 | IV | 1 | 6 | 6 |
The concentration of aztreonam in saliva at 30 minutes after a single 1 g intravenous dose (9 patients) was 0.2 mcg/mL; in human milk at 2 hours after a single 1 g intravenous dose (6 patients), 0.2 mcg/mL, and at 6 hours after a single 1 g intramuscular dose (6 patients), 0.3 mcg/mL; in amniotic fluid at 6 to 8 hours after a single 1 g intravenous dose (5 patients), 2 mcg/mL. The concentration of aztreonam in peritoneal fluid obtained 1 to 6 hours after multiple 2 g intravenous doses ranged between 12 mcg/mL and 90 mcg/mL in 7 of 8 patients studied.
Aztreonam given intravenously rapidly reaches therapeutic concentrations in peritoneal dialysis fluid; conversely, aztreonam given intraperitoneally in dialysis fluid rapidly produces therapeutic serum levels.
Concomitant administration of probenecid or furosemide and aztreonam causes clinically insignificant increases in the serum levels of aztreonam. Single-dose intravenous pharmacokinetic studies have not shown any significant interaction between aztreonam and concomitantly administered gentamicin, nafcillin sodium, cephradine, clindamycin, or metronidazole. No reports of disulfiram-like reactions with alcohol ingestion have been noted; this is not unexpected since aztreonam does not contain a methyl-tetrazole side chain.
Microbiology
Mechanism of Action
Aztreonam is a bactericidal agent that acts by inhibition of bacterial cell wall synthesis. Aztreonam has activity in the presence of some beta-lactamases, both penicillinases and cephalosporinases, of Gram-negative and Gram-positive bacteria.
Mechanism of Resistance
Resistance to aztreonam is primarily through hydrolysis by beta-lactamase, alteration of penicillin-binding proteins (PBPs), and decreased permeability.
Interaction with Other Antimicrobials
Aztreonam and aminoglycosides have been shown to be synergistic in vitro against most strains of P. aeruginosa, many strains of Enterobacteriaceae, and other Gram-negative aerobic bacilli.
Aztreonam has been shown to be active against most strains of the following microorganisms, both in vitro and in clinical infections as described in the INDICATIONS AND USAGE section.
Aerobic Gram-negative microorganisms:
- Citrobacter species
- Enterobacter species
- Escherichia coli
- Haemophilus influenzae (including ampicillin-resistant and other penicillinase-producing strains)
- Klebsiella oxytoca
- Klebsiella pneumoniae
- Proteus mirabilis
- Pseudomonas aeruginosa
- Serratia species
The following in vitro data are available, but their clinical significance is unknown. At least 90% of the following microorganisms exhibit an in vitro minimum inhibitory concentration (MIC) less than or equal to the susceptible breakpoint for aztreonam. However, the efficacy of aztreonam in treating clinical infections due to these microorganisms has not been established in adequate and well-controlled clinical trials.
Aerobic Gram-negative microorganisms:
- Aeromonas hydrophila
- Morganella morganii
- Neisseria gonorrhoeae (including penicillinase-producing strains)
- Pasteurella multocida
- Proteus vulgaris
- Providencia stuartii
- Providencia rettgeri
- Yersinia enterocolitica
Aztreonam and aminoglycosides have been shown to be synergistic in vitro against most strains of P. aeruginosa, many strains of Enterobacteriaceae, and other Gram-negative aerobic bacilli.
Alterations of the anaerobic intestinal flora by broad-spectrum antibiotics may decrease colonization resistance, thus permitting overgrowth of potential pathogens, eg, Candida and Clostridium species. Aztreonam has little effect on the anaerobic intestinal microflora in in vitro studies. Clostridium difficile and its cytotoxin were not found in animal models following administration of aztreonam (see ADVERSE REACTIONS: Gastrointestinal).
Find AZTREONAM medical information:
Find AZTREONAM medical information:
AZTREONAM Quick Finder
Health Professional Information
Clinical Pharmacology
CLINICAL PHARMACOLOGY
Single 30-minute intravenous infusions of 500 mg, 1 g, and 2 g doses of aztreonam for injection in healthy subjects produced aztreonam peak serum levels of 54 mcg/mL, 90 mcg/mL, and 204 mcg/mL, respectively, immediately after administration; at 8 hours, serum levels were 1 mcg/mL, 3 mcg/mL, and 6 mcg/mL, respectively (Figure 1). Single 3-minute intravenous injections of the same doses resulted in serum levels of 58 mcg/mL, 125 mcg/mL, and 242 mcg/mL at 5 minutes following completion of injection.
Serum concentrations of aztreonam in healthy subjects following completion of single intramuscular injections of 500 mg and 1 g doses are depicted in Figure 1; maximum serum concentrations occur at about 1 hour. After identical single intravenous or intramuscular doses of aztreonam for injection, the serum concentrations of aztreonam are comparable at 1 hour (1.5 hours from start of intravenous infusion) with similar slopes of serum concentrations thereafter.
 |
The serum levels of aztreonam following single 500 mg or 1 g (intramuscular or intravenous) or 2 g (intravenous) doses of aztreonam for injection exceed the MIC90 for Neisseria sp., Haemophilus influenzae, and most genera of the Enterobacteriaceae for 8 hours (for Enterobacter sp., the 8-hour serum levels exceed the MIC for 80% of strains). For Pseudomonas aeruginosa, a single 2 g intravenous dose produces serum levels that exceed the MIC90 for approximately 4 to 6 hours. All of the above doses of aztreonam for injection result in average urine levels of aztreonam that exceed the MIC90 for the same pathogens for up to 12 hours.
When aztreonam pharmacokinetics were assessed for adult and pediatric patients, they were found to be comparable (down to 9 months old). The serum half-life of aztreonam averaged 1.7 hours (1.5 to 2) in subjects with normal renal function, independent of the dose and route of administration. In healthy subjects, based on a 70 kg person, the serum clearance was 91 mL/min and renal clearance was 56 mL/min; the apparent mean volume of distribution at steady-state averaged 12.6 liters, approximately equivalent to extracellular fluid volume.
In elderly patients, the mean serum half-life of aztreonam increased and the renal clearance decreased, consistent with the age-related decrease in creatinine clearance. The dosage of aztreonam for injection should be adjusted accordingly (see DOSAGE AND ADMINISTRATION: Renal Impairment in Adult Patients).
In patients with impaired renal function, the serum half-life of aztreonam is prolonged (see DOSAGE AND ADMINISTRATION: Renal Impairment in Adult Patients). The serum half-life of aztreonam is only slightly prolonged in patients with hepatic impairment since the liver is a minor pathway of excretion.
Average urine concentrations of aztreonam were approximately 1,100 mcg/mL, 3,500 mcg/mL, and 6,600 mcg/mL within the first 2 hours following single 500 mg, 1 g, and 2 g intravenous doses of aztreonam for injection (30-minute infusions), respectively. The range of average concentrations for aztreonam in the 8- to 12-hour urine specimens in these studies was 25 to 120 mcg/mL. After intramuscular injection of single 500 mg and 1 g doses of aztreonam for injection, urinary levels were approximately 500 mcg/mL and 1,200 mcg/mL, respectively, within the first 2 hours, declining to 180 mcg/mL and 470 mcg/mL in the 6- to 8-hour specimens. In healthy subjects, aztreonam is excreted in the urine about equally by active tubular secretion and glomerular filtration. Approximately 60% to 70% of an intravenous or intramuscular dose was recovered in the urine by 8 hours. Urinary excretion of a single parenteral dose was essentially complete by 12 hours after injection. About 12% of a single intravenous radiolabeled dose was recovered in the feces. Unchanged aztreonam and the inactive beta-lactam ring hydrolysis product of aztreonam were present in feces and urine.
Intravenous or intramuscular administration of a single 500 mg or 1 g dose of aztreonam for injection every 8 hours for 7 days to healthy subjects produced no apparent accumulation of aztreonam or modification of its disposition characteristics; serum protein binding averaged 56% and was independent of dose. An average of about 6% of a 1 g intramuscular dose was excreted as a microbiologically inactive open beta-lactam ring hydrolysis product (serum half-life approximately 26 hours) of aztreonam in the 0- to 8-hour urine collection on the last day of multiple dosing.
Renal function was monitored in healthy subjects given aztreonam; standard tests (serum creatinine, creatinine clearance, BUN, urinalysis, and total urinary protein excretion) as well as special tests (excretion of N-acetyl-β-glucosaminidase, alanine aminopeptidase, and β2-microglobulin) were used. No abnormal results were obtained.
Aztreonam achieves measurable concentrations in the following body fluids and tissues:
| Fluid or Tissue | Dose (g) | Route | Hours Post-injection | Number of Patients | Mean Concentration (mcg/mL or mcg/g) |
|---|---|---|---|---|---|
| |||||
| Fluids | |||||
| bile | 1 | IV | 2 | 10 | 39 |
| blister fluid | 1 | IV | 1 | 6 | 20 |
| bronchial secretion | 2 | IV | 4 | 7 | 5 |
| cerebrospinal fluid (inflamed meninges) | 2 | IV | 0.9 to 4.3 | 16 | 3 |
| pericardial fluid | 2 | IV | 1 | 6 | 33 |
| pleural fluid | 2 | IV | 1.1 to 3 | 3 | 51 |
| synovial fluid | 2 | IV | 0.8 to 1.9 | 11 | 83 |
| Tissues | |||||
| atrial appendage | 2 | IV | 0.9 to 1.6 | 12 | 22 |
| endometrium | 2 | IV | 0.7 to 1.9 | 4 | 9 |
| fallopian tube | 2 | IV | 0.7 to 1.9 | 8 | 12 |
| fat | 2 | IV | 1.3 to 2 | 10 | 5 |
| femur | 2 | IV | 1 to 2.1 | 15 | 16 |
| gallbladder | 2 | IV | 0.8 to 1.3 | 4 | 23 |
| kidney | 2 | IV | 2.4 to 5.6 | 5 | 67 |
| large intestine | 2 | IV | 0.8 to 1.9 | 9 | 12 |
| liver | 2 | IV | 0.9 to 2 | 6 | 47 |
| lung | 2 | IV | 1.2 to 2.1 | 6 | 22 |
| myometrium | 2 | IV | 0.7 to 1.9 | 9 | 11 |
| ovary | 2 | IV | 0.7 to 1.9 | 7 | 13 |
| prostate | 1 | IM | 0.8 to 3 | 8 | 8 |
| skeletal muscle | 2 | IV | 0.3 to 0.7 | 6 | 16 |
| skin | 2 | IV | 0 to 1 | 8 | 25 |
| sternum | 2 | IV | 1 | 6 | 6 |
The concentration of aztreonam in saliva at 30 minutes after a single 1 g intravenous dose (9 patients) was 0.2 mcg/mL; in human milk at 2 hours after a single 1 g intravenous dose (6 patients), 0.2 mcg/mL, and at 6 hours after a single 1 g intramuscular dose (6 patients), 0.3 mcg/mL; in amniotic fluid at 6 to 8 hours after a single 1 g intravenous dose (5 patients), 2 mcg/mL. The concentration of aztreonam in peritoneal fluid obtained 1 to 6 hours after multiple 2 g intravenous doses ranged between 12 mcg/mL and 90 mcg/mL in 7 of 8 patients studied.
Aztreonam given intravenously rapidly reaches therapeutic concentrations in peritoneal dialysis fluid; conversely, aztreonam given intraperitoneally in dialysis fluid rapidly produces therapeutic serum levels.
Concomitant administration of probenecid or furosemide and aztreonam causes clinically insignificant increases in the serum levels of aztreonam. Single-dose intravenous pharmacokinetic studies have not shown any significant interaction between aztreonam and concomitantly administered gentamicin, nafcillin sodium, cephradine, clindamycin, or metronidazole. No reports of disulfiram-like reactions with alcohol ingestion have been noted; this is not unexpected since aztreonam does not contain a methyl-tetrazole side chain.
Microbiology
Mechanism of Action
Aztreonam is a bactericidal agent that acts by inhibition of bacterial cell wall synthesis. Aztreonam has activity in the presence of some beta-lactamases, both penicillinases and cephalosporinases, of Gram-negative and Gram-positive bacteria.
Mechanism of Resistance
Resistance to aztreonam is primarily through hydrolysis by beta-lactamase, alteration of penicillin-binding proteins (PBPs), and decreased permeability.
Interaction with Other Antimicrobials
Aztreonam and aminoglycosides have been shown to be synergistic in vitro against most strains of P. aeruginosa, many strains of Enterobacteriaceae, and other Gram-negative aerobic bacilli.
Aztreonam has been shown to be active against most strains of the following microorganisms, both in vitro and in clinical infections as described in the INDICATIONS AND USAGE section.
Aerobic Gram-negative microorganisms:
- Citrobacter species
- Enterobacter species
- Escherichia coli
- Haemophilus influenzae (including ampicillin-resistant and other penicillinase-producing strains)
- Klebsiella oxytoca
- Klebsiella pneumoniae
- Proteus mirabilis
- Pseudomonas aeruginosa
- Serratia species
The following in vitro data are available, but their clinical significance is unknown. At least 90% of the following microorganisms exhibit an in vitro minimum inhibitory concentration (MIC) less than or equal to the susceptible breakpoint for aztreonam. However, the efficacy of aztreonam in treating clinical infections due to these microorganisms has not been established in adequate and well-controlled clinical trials.
Aerobic Gram-negative microorganisms:
- Aeromonas hydrophila
- Morganella morganii
- Neisseria gonorrhoeae (including penicillinase-producing strains)
- Pasteurella multocida
- Proteus vulgaris
- Providencia stuartii
- Providencia rettgeri
- Yersinia enterocolitica
Aztreonam and aminoglycosides have been shown to be synergistic in vitro against most strains of P. aeruginosa, many strains of Enterobacteriaceae, and other Gram-negative aerobic bacilli.
Alterations of the anaerobic intestinal flora by broad-spectrum antibiotics may decrease colonization resistance, thus permitting overgrowth of potential pathogens, eg, Candida and Clostridium species. Aztreonam has little effect on the anaerobic intestinal microflora in in vitro studies. Clostridium difficile and its cytotoxin were not found in animal models following administration of aztreonam (see ADVERSE REACTIONS: Gastrointestinal).
Resources
Didn’t find what you were looking for? Contact us.
Chat online with Pfizer Medical Information regarding your inquiry on a Pfizer medicine.
*Speak with a Pfizer Medical Information Professional regarding your medical inquiry. Available 9AM-5Pm ET Monday to Friday; excluding holidays.
Submit a medical question for Pfizer prescription products.
Report Adverse Event
To report an adverse event related to the Pfizer-BioNTech COVID-19 Vaccine, and you are not part of a clinical trial* for this product, click the link below to submit your information:
Pfizer Safety Reporting Site*If you are involved in a clinical trial for this product, adverse events should be reported to your coordinating study site.
If you cannot use the above website, or would like to report an adverse event related to a different Pfizer product, please call Pfizer Safety at (800) 438-1985.
You may also contact the U.S. Food and Drug Administration (FDA) directly to report adverse events or product quality concerns either online at www.fda.gov/medwatch or call (800) 822-7967.